Mum Rage and the Neurodivergent Mother: Why It Hits Differently
The first time I screamed at one of my children, I did not recognise the sound that came out of me.
I was in the thick of motherhood. I had survived a traumatic twin birth, a major depressive episode, a long burnout, and the slow-dawning realisation that I was probably autistic. By the time my third daughter was old enough to be in the room when the rage arrived, I had a vocabulary for most of what was happening to me, all except for that. The shame afterwards was the kind that follows you into the next room. The deeper, more frightening shame of I do not recognise the woman who just did that.
If you are reading this somewhere quiet, like the bathroom, the car, the corner of the kitchen, and what is loudest right now is not the rage but the shame, this post is for you. Whether you have a formal diagnosis of ADHD or autism, whether you are still piecing it together, whether you have always identified as an empath or a highly sensitive person, what just happened has a mechanism, a clinical explanation, and a name.
Three Vocabularies, One Nervous System Event
The phenomenon you have just experienced sits at the intersection of three different bodies of clinical research that, until very recently, have not spoken to each other.
The general parenting literature calls it mum rage or maternal rage: a sudden, intense outburst of anger that mothers report most often in the postpartum period and the early years of caring for small children. The general research treats it as a symptom of postpartum mood disorders or unmet needs, and there is genuine evidence that it is common: a 2022 Canadian survey found that 31% of postpartum women reported intense anger.
The ADHD literature calls it ADHD rage: a sudden, intense anger outburst linked to ADHD's underlying difficulty with emotional regulation. Although it does not appear as a formal DSM-5 diagnosis, emotional dysregulation is now recognised by clinicians as a core feature of attention deficit disorder in adolescents and adults. Around 34–70% of adults with ADHD report experiencing rapid, intense mood shifts, including impulsivity and emotional outbursts that feel harder to control than in neurotypical people.
The autism literature uses different language entirely; it names meltdown and shutdown: two distinct overwhelm responses that occur when an autistic person can no longer process the demands placed on them. A 2022 survey of perinatal experiences found that autistic women were significantly more likely than non-autistic women to have experienced a meltdown during the perinatal period (29% vs. 17%) and a shutdown (38% vs. 8%). The shutdown rate is nearly five times higher.
For a mother with ADHD, autism, or both, these are the same event described in three different vocabularies.
This post integrates them. There is currently no published research that names neurodivergent mum rage as its own phenomenon; the components have been studied separately. The integration of what happens when ADHD, difficulty regulating emotions, autistic sensory-related and processing differences, and the specific neurological demands of becoming a mother collide in the same body is what I explore here. Neurodiversity research is beginning to close this gap, but the clinical literature has not yet caught up with the lived experience.
What Mum Rage Feels Like From the Inside
There is a particular experience that ADHD and autistic mothers describe again and again. It goes like this:
One moment I was fine. The next, I was screaming.
Not gradually. Not with a warning. A spiral that burst from zero to a hundred in what felt like a single second.
The physical experience carries a recognisable pattern. A sudden surge of heat, often in the chest or face. The sensation of something exploding outward that you cannot contain. Hands that clench without your permission. A voice that comes out louder, sharper, and stranger than you knew you were capable of. The feeling of stepping outside yourself and watching from a distance, then followed by a crash. Trembling. Cold sweats. A wave of guilt so thick it is almost physical.
For mothers with ADHD or autism, the pattern often includes additional features. The way that sensory-related information is perceived can become painful. Incoming sound or touch becomes impossible to filter. The room itself can feel hostile. Some women describe what feels like a brief blackout, a few seconds where awareness narrows so tightly that they cannot remember exactly what they said. Others describe the opposite: hyper-clarity, where every sound and movement registers at painful intensity.
Whatever the specific pattern, the core experience is consistent. It comes out of nowhere. It feels reactive, uncontrollable, and impossible to step away from in the moment. And it is followed by a particular shame that does not lift cleanly.
What Just Happened — The Mechanism in Plain Language
The event you have just experienced is a specific neurological pattern; it is a rapid escalation that occurs when the early-warning system most people rely on is not functioning the way it normally does in a neurotypical brain. Some practitioners describe this as an emotional spike.
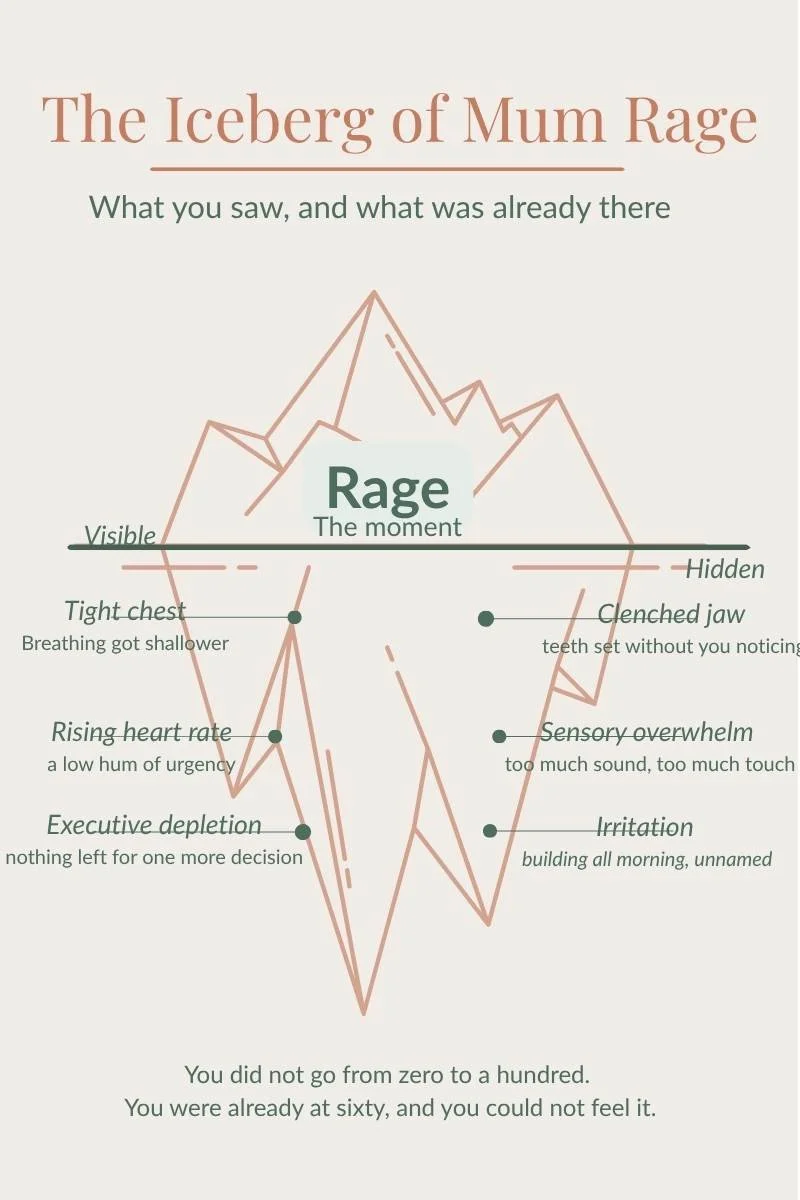
For autistic and ADHD women, the internal sensing system, which is called interoception, is often quieter than average. Your body is sending signals all day. They are simply not landing in awareness with enough clarity to act on. So you move through frustration, sensory overload, executive depletion, and accumulating irritation without consciously registering any of it. You think you are fine. Until you are not.
This is closely connected to alexithymia. Best described as difficulty in identifying and naming what you are feeling from the inside. A 2024 meta-analysis of 32 studies and nearly 8,000 participants found that alexithymia reflects a broader difficulty with interoception, not just a feelings vocabulary issue. The body signals that should provide the early warning, like the tight chest, the clenched jaw, the rising heart rate, the low hum of irritation, do not come through clearly. All that arrives is the rage.
The Hampton survey of perinatal experiences supports this directly: autistic women were significantly more likely to report changes in their interoception (69% vs. 42% reported a change) and proprioception (38% vs. 15%). The interoceptive gap that drives the rage is documented in the perinatal context specifically.
You did not go from zero to a hundred. You were already at sixty, and you could not feel it.
Why Motherhood Is the Trigger
If you are reading this, thinking — but I never used to be like this — there is a reason. The reason has very little to do with becoming a worse person.
Many women with this profile retrospectively recognise that what is happening now follows a pattern that has been present for years. The flooding, the shutting down, the sense of being overtaken by something larger than yourself, these may have been present in adolescence too. What has changed is that you are responsible for a small person who depends on you, and the same brain-based event lands very differently when it does. The rage that frightened only you at thirteen now frightens a child watching from the doorway.
Four mechanisms turn everyday challenges with regulation into the specific phenomenon of mum rage.
1. Hormonal volatility
Oestrogen is understood to influence dopamine regulation, which affects attention, motivation, and emotional regulation. Across the menstrual cycle, in pregnancy, and most dramatically in the postpartum period, oestrogen levels shift in ways that destabilise a brain that already struggles with impulse control and executive dysfunction. ADHD and autistic features sharpen. Sensory tolerance drops. Emotional outbursts increase. The threshold for overwhelm lowers. The pattern is increasingly recognised in the research, and it is not in your head. It is in your hormones.
2. Masking collapse
The sustained effort of suppressing or concealing ADHD and autistic traits to appear neurotypical comes with a price, and it is a high one. A 2024 study found that people with ADHD reported significantly higher camouflaging than neurotypical groups, particularly on day-to-day masking behaviours. Motherhood strips the capacity to maintain it. When the mask collapses under depletion, what is underneath is a brain running at overcapacity, in constant overstimulation, with an early-warning system already impaired.
3. Sensory overload as fight response
A qualitative study of autistic mothers found that 96% of autistic individuals experience sensory processing differences. Parenting presents with extreme demands like constant touch, unpredictable sound, lack of sleep, the loss of recovery time and quiet space, many autistic women relied on before becoming a mother. When this system has been overloaded long enough, it responds differently to a neurotypical system. It moves into fight. The rage that follows is what happens when a sensory-overloaded brain runs out of capacity to do anything else.
4. Executive depletion
The interaction between autism's need for sameness and ADHD's executive dysregulation creates what one of my clients once described as being completely paralysed by the thing I most want to do. Add the relentless decision-making demands of caring for a small person. Every feeding, every nappy change, every transition requires planning, sequencing, and follow-through. The executive system moves into chronic overdraft. Emotional regulation is dependent on executive function, and when executive function is depleted, the emotional braking system loses its primary mechanism.
What for many women shows up as a postpartum meltdown is often better understood as an autistic or ADHD shutdown happening in a body that has nowhere left to discharge it. One autistic mother in a 2021 qualitative study described her postpartum experience as a prolonged meltdown caused by the loss of every coping strategy she had ever relied on, uncertain whether what she had lived through was postnatal depression or something different. Many mothers with ADHD and autism will recognise this uncertainty.
The Autistic Mother Experience Specifically
Within the broader picture of mum rage in AuDHD and autistic mothers, the autistic mother's experience deserves its own naming. The research base is small but clear.
Autistic women are significantly more likely to experience meltdowns and shutdowns in the perinatal period, and both at rates roughly twice as high as non-autistic women, and with shutdown rates nearly five times higher. The reasons are structural and predictable.
The autistic brain processes more sensory input, more intensely, with reduced ability to filter or habituate. Pre-motherhood, most autistic women had built, often unconsciously, an entire architecture of recovery: time alone, predictable routines, sensory management, control over the rhythm of social demand. Pregnancy disrupts all of it. The postpartum period demolishes it. Some women withdraw entirely into themselves during this phase, and what looks like depression from the outside is often a sustained shutdown from within.
Add to this the heightened rejection-sensitive dysphoria that affects many women with ADHD and autism: a partner's sigh, a baby who will not settle, a health visitor's tone, all of these can register through the RSD alarm as rejection or failure, which then fires through a postpartum body already in depletion. The inability to stay calm that follows is not disproportionate to what was experienced internally. It is disproportionate only to what actually happened.
If you would like to read more about how RSD overlaps with birth trauma in ADHD and autistic mothers, the pillar post on Rejection Sensitive Dysphoria in motherhood goes deeper.
How Mum Rage Lands on the People Around You
The rage does not happen in isolation. It happens in front of children, partners, and sometimes extended family, and the impact on those relationships is one of the things that makes mum rage so painful to live with.
For children, the pattern matters more than the individual incident. Children are not damaged by parents who lose their temper occasionally. They are affected by environments where rage is constant, unpredictable, and never followed by repair. A single rage event followed by a moment to pause and regulate emotions, so you can then proceed with a calm, age-appropriate repair conversation, is not the same as a household where the rage simmers daily. A repair conversation does not need to be long or complex: what happened was not your fault, I was overwhelmed, I am sorry I shouted, is enough. The repair is what protects the relationship. And when an apology is given calmly and genuinely, children learn something important: that adults can lose their temper, recognise it, and apologise. You are not supposed to be a perfect mother; you are supposed to be a human who makes mistakes and owns up to them, and models repair to her child.
For partners, the rage often becomes a source of relationship pressure that is hard to name. The non-rage partner may feel walking-on-eggshells exhaustion. The mother may feel that her partner does not understand the depth of what is driving the dysregulation. Resentment can build in both directions. Honest conversation about what is actually happening, which may include, where appropriate, the brain-based mechanism behind it, is often the route through. A partner who understands that the rage comes from an overtaxed brain, not a personal attack, can become an ally in managing anger rather than another source of pressure. Practical support, taking over a transition, reducing sensory demands at a known flashpoint, stepping in before the spike rather than after, is often more useful than any amount of processing after the fact.
The shame around this topic often makes women hide it from everyone. A pattern unspoken is much harder to change than a pattern named and understood.
If you are reading this in or just after a moment of mum rage and you would like something concrete to take away today, the Mum Rage Recovery Map is a free guide written for exactly this moment. It walks you through what just happened, why your body did not warn you, and three things that help in the next hour
Strategies That Help — Managing Anger and Mum Rage
Generic advice about this topic was not written with an ADHD or autistic brain in mind. Sleep when the baby sleeps. Just ask for help. Lower your standards. Every mother finds it hard. For a mother with ADHD or autism in genuine dysregulation, this advice is not just unhelpful; it can be actively harmful, leading to further isolation and increasing feelings of shame. It assumes a brain that responds to rest the way most people's do. It assumes that reaching out feels straightforward. It assumes the difficulty is proportional to a neurotypical mother's, only turned up slightly.
Mum rage in an ADHD or autistic brain is a different kind of hard. What helps is different, too.
The interventions that work are divided into upstream and downstream categories. Both matter. The upstream category matters more.
Upstream: building the early-warning system
If the rage arrives without warning because the warning signals are not being received, the most leveraged intervention is upstream, building interoceptive awareness so the body's signals become legible before the crisis point. Rather than trying to label emotions, the work is to scan the body and identify physical sensations: where there is tightness, where there is heat, where there is nothing. Restoring the body–emotion link is what rebuilds the foundation for self-regulation. It takes time. It works. It makes what currently feels unmanageable manageable, not by removing the difficulty, but by catching it earlier.
The Mum Rage Recovery Map and the Body Signal Tracker (releasing as the next free resource on this site) are both designed to support this upstream work specifically.
Environment modification before behaviour change
Burnout is the result of too much stress and insufficient resources to cope with it. For mothers with ADHD or autism, the most effective initial intervention is rarely a new skill; it is reducing the load. Sensory load. Decision load. Social load. Reducing demands, simplifying routines, and protecting genuine recovery windows is structural work that reduces the frequency of the rage before any therapeutic work on the rage itself begins. Setting boundaries as an ADHD mother is the practical companion piece on this.
Concrete coping strategies that often help:
Identify your sensory triggers and reduce them where possible. Lower lighting, noise-cancelling headphones, soft clothing, fewer mirrors and reflections.
Normalise asking for true recovery time, not just a break. Twenty minutes alone in a quiet room is different from twenty minutes with the baby on the other side of a thin wall.
Unmask when possible. Enlist the help of a family member you identify as safe, someone you can be yourself around, who can offer practical support without adding social demand.
Build pattern recognition into the week. Notice which days, hours, or transitions consistently bring you closest to the spike. Adjust the structure where you can.
Reconnect with the coping strategies you used before motherhood. Many were stripped away by the early postpartum period. Some can come back, in adapted form.
DBT components
Dialectical Behaviour Therapy has solid evidence for emotional dysregulation in adult ADHD. Specifically useful for mum rage are chain analysis, which identifies the sequence of events, thoughts, and feelings leading up to an outburst, and opposite action, practising a pause before reacting, rather than allowing the urge to lash out to drive behaviour. These are concrete, teachable, and compatible with an ADHD or autistic brain when framed correctly.
CBT — useful, with one caveat
Standard cognitive behavioural therapy assumes the person can identify and label their emotional state before responding to it. For women with ADHD and alexithymia, this assumption breaks down. The work of reframing thought patterns only becomes available once there is enough interoceptive awareness to notice what is happening before the spike. CBT works best after some interoceptive foundation has been built, or when adapted specifically for alexithymic presentation. Ask any therapist before starting work whether they have experience adapting their approach for ADHD or autistic clients.
Trauma-informed support
For women where mum rage is entangled with birth trauma, which the research suggests is significantly more common in women with ADHD and autism, the anger is partly a trauma response, not purely a dysregulation response. Trauma-informed and somatic approaches are needed alongside any skills-based work.
Perinatal-specific support
The 2024 systematic review on the neurodivergent perinatal experience was clear: generic perinatal support is documented as inadequate for women with ADHD and autism. What is needed is constructive, practical support that is specifically perinatal and specifically neuro-affirming. That is what I offer through Perinatal Counselling.
Frequently Asked Questions
Is mum rage the same as ADHD rage?
Not exactly. ADHD rage is the broader structural condition — the emotional dysregulation that is now recognised as a core feature of ADHD symptoms, affecting roughly 70% of adults with the condition, and sometimes comorbid with autistic traits. Mum rage is one specific context in which ADHD rage manifests: the postpartum and early-parenting context, where hormonal shifts, sleep deprivation, sensory demands, and the witness pressure of being watched by your child all amplify the underlying dysregulation. A woman with ADHD can experience this rage without being a mother. A mother with ADHD or autism who experiences this is, in clinical terms, having emotional dysregulation in a uniquely demanding context.
What is the difference between mum rage and postpartum rage?
The two terms are often used interchangeably, but they are not identical. Postpartum rage refers specifically to anger that emerges in the first year after birth, most often discussed as a symptom of perinatal mood and anxiety disorders. Mum rage is the broader umbrella term for maternal anger across the parenting years — including, but not limited to, the postpartum period. Many mothers experience both: postpartum rage that begins in the early months and continues to surface as mum rage years later when the structural pressures of parenting persist. For mothers with ADHD and autism specifically, the underlying mechanism tends to be consistent across both phases.
How is mum rage different from postpartum depression?
They can overlap — irritability is a recognised feature of postpartum depression, and approximately one in four postpartum women experience some form of postpartum mental health condition. The two are distinct, however. Postpartum depression involves persistent low mood, loss of interest, and often guilt or feelings of worthlessness. Mum rage is acute and explosive — a sudden spike of anger that feels uncontrollable in the moment and is followed by intense shame. They can co-occur. Both deserve attention. A perinatal mental health practitioner can help you distinguish them.
Is what I am experiencing an autistic meltdown or shutdown?
For autistic mothers specifically, yes — what is often called mum rage is, in a meaningful proportion of cases, what the autism literature calls a meltdown (an externalised overwhelm response involving expression and discharge) or a shutdown (an internalised response involving withdrawal and reduced functioning). The 2022 perinatal experiences survey found these occur at significantly higher rates in autistic mothers than in non-autistic mothers. Whichever term you use, the underlying event is the same, but the language can change the kind of support that helps.
Why does mum rage feel worse when my child is the trigger?
Several factors converge. The witness pressure: your child is watching, and your brain registers this. The maternal-instinct override conflict: the pull to protect and the rage spike occupying the same body. The shame architecture: the cultural mythology of motherhood makes the rage feel like a deeper failure than it would in any other context. And, for many mothers with ADHD and autism, sensory triggers from the child, specifically, like touch, sound, unpredictability, that overwhelm the brain in a particular way. None of these means you love your child less. They mean that mothering is structurally demanding for a brain like yours.
Can mum rage harm my child?
Rage frightens children, and repeated rage without repair can affect a child's sense of safety. What matters alongside the rage is what comes after. Repair conversations, which can only take place once the emotional system has come down, are protective. Children are not damaged by parents who lose their temper occasionally. They are affected by environments where rage is constant, unpredictable, and never followed by repair. If you are concerned about how often the rage is happening or how it is landing on your child, that is exactly the kind of thing worth talking through with a perinatal counsellor or therapist.
Do I need an ADHD or autism diagnosis before I can get help?
A formal diagnosis can open access to specific accommodations and services, and many women find it validating, but it is not a prerequisite for support. You can be undiagnosed and still access counselling, still begin to understand your ADHD symptoms, and still start making changes that reduce overwhelm. If you recognise yourself in this post, support can begin wherever you are right now.
When should I seek professional help for mum rage?
Several signals warrant professional support: when the rage is happening frequently and you cannot identify what is driving it; when you are frightened of what might happen during an outburst; when it is affecting your relationship with your child or partner in a sustained way; when it sits alongside other symptoms like persistent low mood, sleep difficulties, or intrusive thoughts; or when it is connected to unresolved birth trauma. A perinatal counsellor who understands ADHD and autism is the most direct route. Your GP can also refer you to local mental health services. If you are in crisis or feel at risk of harming yourself or your child, contact emergency services or your local crisis line immediately.
A Final Note
Understanding that you are AuDHD, have ADHD, are autistic, or simply have a brain that has always worked this way does not make the rage acceptable. It means there is a reason behind it. There is a difference between the two, and the difference matters.
The rage is the visible part of an invisible mechanism that has been building for hours, days, sometimes weeks, in a body that could not tell you it was happening. Identifying the mechanism is the first part of changing what happens next time — and reframing it from a character flaw into a brain-based pattern is what makes the work of change actually possible.
You are a woman whose brain processes the world differently, and who, on top of that, is doing one of the most demanding jobs a human can do, often without enough sleep, often without enough support, often without language for what is happening inside her. That is a context that requires the right kind of help.
If you would like to explore what neuro-affirming perinatal counselling looks like for you, a free 30-minute discovery call is a good place to start. No commitment, no pressure.